Recovery That Meets You Where You Are
Whether you're reaching out for yourself, someone you care about, or a client in need of support, Cenikor is here to help you take the next step. With flexible, evidence-based care and a commitment to serving everyone, we make recovery more accessible—and more sustainable.
Start the ConversationKey Takeaways
- Summer removes the school-year scaffolding of teachers, coaches, and routines that quietly monitor teens, leaving parents as the primary people noticing shifts in mood, sleep, and behavior.
- More teens try alcohol and marijuana for the first time in June and July than any other months, with over 11,000 daily first-time alcohol users in summer 5.
- Sleeping in is normal, but sleeping through plans a teen made themselves — jobs, pool days, family events — signals a flatness worth taking seriously 9.
- One new friend is growth; rotating through three friend groups in six weeks with vague answers and unfamiliar pickups points to a teen reorganizing their social world around something hidden 9.
- A messy room is teenage life, but a locked door paired with new smells, eye drops, weight changes, and declining hygiene is the cluster federal guidance treats as warning signs 6.
- Bloodshot eyes, mismatched pupils, sudden weight shifts, neglected hygiene, shaky hands, and flipped sleep schedules stack into a physical picture the body shows when a teen won’t talk.
- Family history of substance use, thinner parental monitoring, using friends, weak school belonging, and ongoing mood struggles raise risk and should sharpen — not paralyze — how you read warning signs 1.
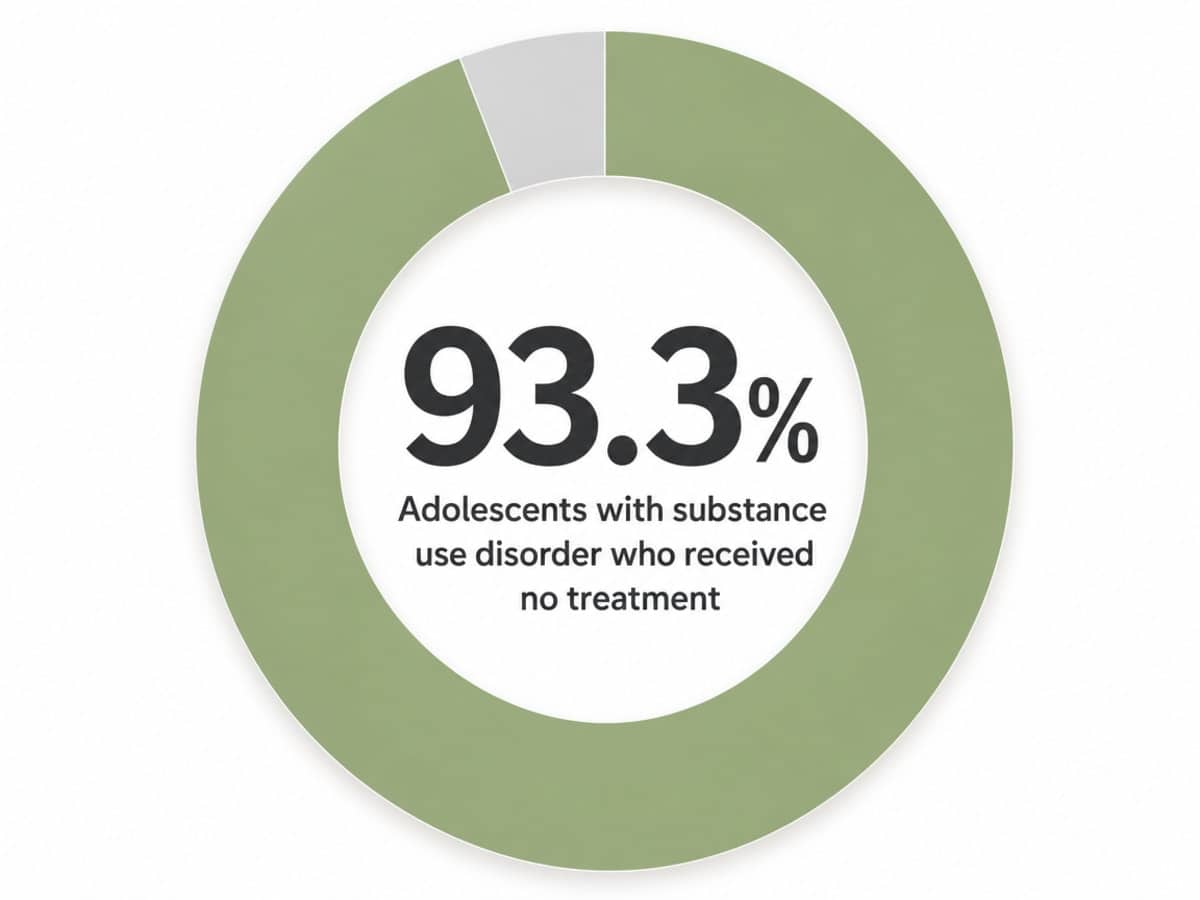
- Roughly 1.7 million U.S. adolescents met criteria for a substance use disorder in 2024, and 93.3% received no treatment that year, often because families waited for certainty 12.
- Write down concrete observations, call an intake team to match outpatient, partial hospitalization, or residential care to your teen’s actual needs, and tell one other adult so you’re not carrying it alone.
What You’re Noticing in June Isn’t Nothing
You’ve been watching your kid for weeks now. The eye contact is shorter. The bedroom door stays closed longer. There’s a new flatness in their voice, or a new edge, and you keep telling yourself it’s hormones, or end-of-school stress, or just being fifteen. Maybe it is. But you opened this article, which means some part of you already knows the answer isn’t that simple.
Here’s what to hold onto first: noticing is not overreacting. Parents who pick up on early changes in personality, mood, and habits are doing the exact thing the research says matters most for catching teen substance use before it grows roots 9. You are not paranoid for paying attention. You are paying attention because something shifted, and you live with this person every day, and you can tell.
Summer is when those shifts get loud. The school-year scaffolding that used to mask the smaller signs — the morning bus, the coach’s text, the teacher’s email about a missed assignment — is gone. What’s left is your gut and your eyes.
This piece will help you sort the normal teenage weirdness from the warning signs that deserve a phone call. Not next semester. This week, if it comes to that.
Why Summer Pulls the Curtain Back
The Scaffolding That Disappears in June
Think about what your teen’s day looked like in April. There was a wake-up time, because the bus came at 7:14. There was a teacher who noticed when they didn’t show up to second period. There was a coach who texted you when they missed practice, a counselor who flagged the failing grade, a friend’s mom who mentioned seeing them at the mall on a Tuesday afternoon. None of that was perfect, but all of it was watching.
In June, that whole system goes quiet. No grades coming home. No attendance reports. No teacher email about the missing essay. The people who used to share the load of noticing your kid are off for the summer too.
What you’re left with is your living room, your driveway, and your gut. Most of the warning signs the research describes — secrecy, deception, mood swings, withdrawal from family routines — are the kind of thing a school year half-hides because everyone is too busy to notice 9. Summer slows the family down enough that you finally see them.
That’s not a bad thing. It’s hard, and it’s lonely, and it can feel like you’re suddenly the only adult paying attention. But the curtain pulling back is what gives you a chance to act early instead of late.
Summer Is When Initiation Spikes
Here’s something that might make your stomach drop, and also might validate what you’ve been feeling: more teens start drinking and using drugs in June and July than in any other months of the year. SAMHSA’s national survey data shows that on a typical day in June or July, more than 11,000 adolescents try alcohol for the first time, compared with an annual daily average of around 7,800. For marijuana, the June and July daily figure climbs above 4,800 new users 5. That’s not a small bump. That’s a season-shaped curve.
The reason is the same scaffolding story from above. When school ends, supervised hours drop. Kids who would never have a chance to drink at 2 p.m. on a Wednesday in March suddenly have whole afternoons with friends, empty houses, older siblings home from college, and pool parties where someone’s parent is conveniently out of town. The opportunity changes, and so does the behavior.
So when you find yourself thinking, “It feels like something changed when school let out” — that’s not in your head. That’s the calendar doing what it does to teenagers every year. The good news is that catching a shift this early, in the season when it’s most likely to start, is exactly the timing that makes early help possible.
Normal Teen Weirdness vs. Warning-Sign Weirdness
Sleeping In vs. Sleeping Through Their Own Plans
Sleeping until 11 a.m. in July is not a warning sign. Teen bodies run on a different clock, and summer lets them finally hit it. If your kid is staying up late watching shows, scrolling, or texting friends, then crashing through the morning, that’s just a teenager in summer.
What’s different is when sleep starts breaking the things they actually wanted. The pool day they begged you to plan, and now they won’t get up for. The lifeguard shift they applied for in April, and now they’re calling in sick to. The cousin’s birthday they were excited about last week, and today they say they’re “too tired” while staring at the ceiling.
Sleeping through obligations is normal. Sleeping through their own joy is not. When a teen stops showing up for the plans they made themselves — especially the social ones — that flatness is worth paying attention to. Pair it with mood swings or a new irritability when you wake them, and you’re looking at the kind of pattern early-detection research treats as a real signal, not just laziness 9.
One New Friend vs. Three Rotating Groups
Teens make new friends in summer. Camp, the job at the snow cone stand, the neighbor’s cousin visiting from Dallas — a fresh face in your kitchen is not a red flag. One new friend, even one you don’t love, is part of growing up.
What to watch for is the cycle. Three different groups in six weeks, each one further from the kids you knew. Names you can’t keep straight. Pickups in cars you’ve never seen, from people who don’t come to the door. Old friends suddenly disappearing from the group chat, and no clear reason why.
The pattern researchers describe in early-detection literature isn’t “new friends.” It’s the deception, secrecy, and mood instability that often travel with a shifting peer group — vague answers about where they were, manipulative or short-tempered reactions when you ask follow-up questions, and a creeping flatness or low mood between social hits 9. One new friend asks you for a ride. Rotating groups means your teen is reorganizing their social world around something they don’t want you to see. That’s the difference.
A Messy Room vs. a Locked Door and a New Smell
A messy room is a teenager. Clothes on the floor, three water glasses on the nightstand, a hoodie that’s been there since May — none of that means anything. Plenty of healthy kids live in a swamp of laundry from June to August, and you can leave that battle for another day.
What’s different is when the room becomes a sealed-off space. The door that used to be cracked is now locked. A towel jammed under it. A fan running at odd hours. New smells you can’t place — incense over something sweet, body spray over something skunky. Eye drops on the dresser that nobody needed last summer. A lighter in a drawer of a kid who doesn’t smoke.
Personality and appearance changes that show up alongside the locked door — poor hygiene, sudden weight changes, bloodshot eyes, a new flatness around the family — are the cluster the Department of Justice’s parent-facing guidance flags as warning signs of use, not just privacy 6. A messy room wants to be left alone. A locked-down room is hiding something. Trust the difference.
What the Body Is Telling You
Behavior tells one story. The body tells another, and it’s often the harder one to argue with.
Start with the eyes. Bloodshot whites in a kid who hasn’t been swimming. Pupils that don’t quite match the lighting in the room — too wide in bright sun, too pinned in a dim kitchen. A glassy distance when they look at you, like they’re listening through water. Eye drops appearing on the bathroom counter is the giveaway most parents catch second, after they’ve already noticed the redness.
Then weight and appetite. A teen who skipped breakfast all spring is one thing. A teen who suddenly can’t stop eating at midnight, or who’s lost ten pounds since Memorial Day without trying, is another. Sudden personality and physical-appearance shifts — weight changes, declining hygiene, a tired face that wasn’t there in May — are the cluster federal parent-facing guidance treats as warning signs of use rather than ordinary growth 6.
Hygiene is the one parents hate to name. The same kid who used to shower twice a day before practice now smells like yesterday’s clothes and a cover-up scent on top. Hair unwashed for a week. Teeth not brushed. A new indifference to how they look in the mirror.
Also watch the small stuff: shaky hands holding a glass, a runny nose with no cold, a bruise they can’t explain, a sleep schedule that flips the clock. None of these alone is proof. Three or four of them stacked on top of behavioral changes is the body telling you what the mouth won’t.
Who Is Most at Risk and Why It Matters
Every teen is capable of trying something this summer. But some kids are walking into June carrying more weight than others, and knowing where your family sits on that spectrum helps you read the signs with the right urgency.
The CDC’s risk-factor research is plain about what tilts the odds. A family history of substance use — a parent, a grandparent, an older sibling who struggled — raises the baseline. So does a stretch of poor parental monitoring, which doesn’t mean you’re a bad parent, just that life got busy and the check-ins got thinner. Add in friends who are already using, a low sense of belonging at school, and ongoing struggles with mood or anxiety, and you’re looking at the cluster of factors that predicts higher risk for high-risk substance use 1.
None of that is destiny. Plenty of kids with three risk factors stacked up never develop a problem, and plenty of kids with none of them still do. What the list gives you is a way to calibrate your worry. If your teen has a parent in recovery, a new friend group you don’t know, and a rough year academically, the same locked door means more than it would in a household with none of those threads.
This isn’t about labeling your family. It’s about giving yourself permission to act sooner if the picture is denser than it looks from the outside.

Why Waiting Costs More Than Acting
Here is the part nobody likes to say out loud: the families who get help early are not the ones who were sure. They are the ones who acted while they were still unsure. They called when the picture was still messy, when their teen still denied everything, when half the relatives were saying it was just a phase. They did not wait for proof. They waited until they had enough worry to pick up the phone, and that turned out to be enough.
Waiting feels safer because it doesn’t require a hard conversation today. It costs less in the short term. But the math changes fast. Adolescent substance use is linked to overdose risk, academic collapse, and a higher likelihood that occasional use becomes a substance use disorder that follows your kid into their twenties 2. Every month a pattern goes unaddressed is a month it gets more familiar to your teen’s brain and body, and a month harder to interrupt.
You are also not alone in noticing — and that is the part that should land hardest. According to the 2024 National Survey on Drug Use and Health, roughly 1.7 million U.S. adolescents met criteria for a substance use disorder, and 93.3% of them received no treatment that year 12. That is not a story about bad parents. That is a story about families who saw something, hesitated, and ran out of summer. Waiting is the most common response. It is also the most expensive.
Acting early does not mean throwing your kid into residential care this weekend. It means making the call, asking the questions, and letting a professional help you figure out what level of support actually fits. The hard part is the call. After that, you have help.
Trusting Your Gut Without Catastrophizing
You are allowed to be worried and wrong. You are also allowed to be worried and right. The job this summer is not to settle that question by yourself in your kitchen at 11 p.m. with a flashlight and a Google search. The job is to take what you’re seeing seriously without letting your imagination sprint to the worst possible ending.
Here’s a way to hold both. Write down what you’ve actually noticed — dates, behaviors, smells, missed plans, the new name you keep hearing. Not as evidence to confront your teen with tonight, but as a record for you. When the noise in your head says “I’m overreacting,” the list will tell you whether you are. When the noise says “My kid is a different person,” the list will tell you whether the changes are stacking or scattered.
One moody Tuesday is a moody Tuesday. Six weeks of locked doors, new friends you’ve never met, falling weight, and a kid who won’t look you in the eye is a pattern. Patterns deserve a phone call. Single bad days deserve a snack and a check-in.
Trusting your gut means honoring what you see without deciding the ending before a professional has helped you read it.
What the Next Step Actually Looks Like
Outpatient, Residential, and Where Teens Fit
When you make the call, the first thing a good team will do is help you figure out what level of care your teen actually needs — not the most intense one, and not the most convenient one, but the one that fits.
Outpatient is the lightest lift. Your teen lives at home and comes in for therapy, group sessions, and support a few times a week. It works when use is early, the home is stable, and your kid still has reasons to stay engaged — a job, a sport, a relationship that’s holding. You stay close to the day-to-day, and so does the clinical team.
Partial hospitalization sits in the middle. More hours, more structure, still sleeping at home. Useful when outpatient isn’t enough but pulling them out of the house feels too steep.
Residential is where teens go when home has stopped being a place where recovery can start. Use has been heavier, longer, or harder to interrupt. The peer group at home is part of the problem. The summer is slipping. Residential gives a teen a full reset — twenty-four-hour structure, daily therapy, and a break from the environment that’s been feeding the pattern.
You don’t have to pick. The intake team picks with you.
Inside a Day at Cenikor’s Odyssey House Houston Teen Program
Residential treatment sounds scarier than it usually looks from the inside. At Cenikor’s Odyssey House in Houston, the teen program runs on a daily rhythm that, on purpose, looks a lot like the structure summer took away.
Mornings start with a wake-up time, breakfast together, and chores — the small accountability pieces a lot of teens have stopped doing at home. From there, the day moves into individual therapy, group sessions with other teens working through the same thing, and education time so your kid doesn’t fall behind on coursework while they’re in care. Afternoons bring skills groups, recreation, and time to actually be a teenager in a setting where nobody is using.
Meals are shared. Sleep is regular. There’s whole-person support built in — physical health, daily routines, and a peer community that knows why everyone is there. Family is part of the work too, with sessions designed to bring you back into the picture as a partner in the recovery, not a bystander to it.
It’s not a punishment, and it’s not a pause button. It’s a place where a teen can put down what they’ve been carrying and learn what life feels like without it.
How to Move From Noticing to Calling This Week
You don’t need a perfect plan. You need three small moves before Sunday.
- Write down what you’ve actually seen — the dates, the friends’ names, the changes in sleep and weight, the locked door, the missed plans. Keep it on your phone. Patterns are easier to read on paper than in your head at midnight.
- Make the call. Cenikor’s Odyssey House in Houston has an intake team that talks to parents every day who sound exactly like you — unsure, scared, hoping they’re wrong. They will help you figure out whether outpatient, partial hospitalization, or residential care fits, and they will not push your kid into more than is needed.
- Tell one other adult — a partner, a sibling, a close friend. You should not be the only person carrying this. Acting early does not mean acting alone, and the families who get help are the ones who stop waiting for certainty before they pick up the phone.
Frequently Asked Questions
How do I know if my teen’s behavior is just a phase or something more serious?
Phases are usually one thing at a time and pass within a few weeks. Warning signs stack. When you see mood swings, secrecy, new friends, falling weight, and a kid who won’t look you in the eye all in the same month, that pattern is what early-detection research treats as a real signal worth a professional conversation 9.
What’s the difference between experimenting and needing rehab?
Experimenting tends to be one incident, an obvious story, and a kid who’s rattled by it. Needing treatment looks like a pattern — repeated use, hidden use, changes in personality and school performance, and use that keeps going even after consequences. A clinical intake team can sort which one you’re seeing better than you can alone at the kitchen table.
Should I search my teen’s room if I suspect drug use?
It’s your house, and your right. But searching alone rarely settles anything — what you find can be denied, explained away, or hidden better next time. A more useful move is writing down what you’ve already noticed and calling an intake team. They’ll tell you whether what you’re seeing is enough to act on without you turning the bedroom upside down first.
What if my teen refuses to admit there’s a problem?
Most teens deny it, especially at first. You don’t need their agreement to make a call or schedule an assessment. Parents are the ones who get treatment started in the majority of teen cases. Your job isn’t to win the argument tonight. It’s to put a professional in the room with your kid so the conversation stops being just yours.
Can my teen miss school for residential treatment, or do we have to wait until summer ends?
Summer is actually the best window — no missed classes, no awkward absences to explain. But teens enter residential care year-round, and programs like Cenikor’s Odyssey House in Houston include education time so coursework doesn’t fall apart. Don’t wait for a calendar reason. Waiting through fall semester for a problem you’re seeing in July usually makes the problem bigger, not smaller 2.
What does a typical day look like in a teen residential program?
At Cenikor’s Odyssey House Houston teen program, days run on structure: wake-up, breakfast, chores, individual therapy, group sessions with other teens, education time, skills groups, recreation, shared meals, regular sleep. Family sessions bring you back into the work. It’s not isolation or punishment — it’s a full daily rhythm built to replace what use was taking up.
References
- Substance Use Among Youth | Reducing Health Risks … – CDC. https://www.cdc.gov/youth-behavior/risk-behaviors/substance-use-among-youth.html
- Characteristics of Alcohol, Marijuana, and Other Drug Use Among …. https://www.cdc.gov/mmwr/volumes/73/wr/mm7305a1.htm
- Youth High-Risk Drug Use – CDC. https://www.cdc.gov/youth-behavior/risk-behaviors/youth-high-risk-drug-use.html
- YRBS Data Summary & Trends Report – CDC. https://www.cdc.gov/yrbs/dstr/index.html
- Monthly Variation in Substance Use Initiation among Adolescents. https://www.samhsa.gov/data/sites/default/files/NSDUH080/NSDUH080/SR080InitiationSubstanceUse2012.htm
- Teens and Drugs Fast Facts – Department of Justice. https://www.justice.gov/archive/ndic/pubs11/12430/index.htm
- Table 3.1, Risk Factors for Adolescent and Young Adult Substance …. https://www.ncbi.nlm.nih.gov/books/NBK424850/table/ch3.t2/
- Adolescent Substance Use Disorders – PMC. https://pmc.ncbi.nlm.nih.gov/articles/PMC11003516/
- Early Detection of Illicit Drug Use in Teenagers – PMC. https://pmc.ncbi.nlm.nih.gov/articles/PMC3257983/
- SAMHSA Releases Annual National Survey on Drug Use and Health. https://www.samhsa.gov/newsroom/press-announcements/20250728/samhsa-releases-annual-national-survey-on-drug-use-and-health
- [PDF] NSDUH Data Brief: Trends in Substance Use among Young Adults. https://www.samhsa.gov/data/sites/default/files/reports/rpt56978/2024-nsduh-data-brief-young-adult.pdf
- [PDF] Highlights for the 2024 National Survey on Drug Use and Health. https://www.samhsa.gov/data/sites/default/files/NSDUH%202024%20Annual%20Release/2024-nsduh-nnr-highlights.pdf
- Teenagers and drugs: MedlinePlus Medical Encyclopedia. https://medlineplus.gov/ency/article/001975.htm
- 2021-2024 NSDUH Data Brief: Trends in Substance Use … – SAMHSA. https://www.samhsa.gov/data/report/21-24-nsduh-data-brief-trends-substance-use-among-young-adults
- Research Review: What Have We Learned About Adolescent … – PMC. https://pmc.ncbi.nlm.nih.gov/articles/PMC5771977/
Recovery Built for Real Life
Recovery doesn't have to feel out of reach. At Cenikor, we provide practical, affordable care designed for real life—whether you're navigating substance use, supporting a loved one, or helping someone find the right level of care.
Explore Your Options

