Recovery That Meets You Where You Are
Whether you're reaching out for yourself, someone you care about, or a client in need of support, Cenikor is here to help you take the next step. With flexible, evidence-based care and a commitment to serving everyone, we make recovery more accessible—and more sustainable.
Start the ConversationKey Takeaways
- Skill Progression Roadmap: Understanding the long term effects of ketamine use takes time. Begin by identifying cognitive shifts (weeks 1-2), progress to recognizing physical warning signs (weeks 3-4), and master intervention strategies (weeks 5-6).
- Essential Tools: Utilize symptom tracking logs, cognitive assessment checklists, and professional wellness evaluations to monitor changes in yourself or your clients.
- Competency Checklist: You are ready to advance when you can distinguish between temporary brain fog and persistent cognitive decline, identify early urinary tract symptoms, and articulate why professional stabilization is more effective than stopping alone.
What Ketamine Does When Use Becomes Chronic: Long Term Effects of Ketamine Use
It might not feel dangerous in the moment—ketamine’s dissociative effects can seem manageable, even controllable at first. But when use becomes chronic, the long term effects of ketamine use create cascading changes in the body and brain that many professionals don’t anticipate until the damage is already underway. Understanding these long-term effects isn’t about fear—it’s about recognizing when patterns have shifted from experimentation to something that requires structured, professional intervention.
When ketamine use becomes a regular pattern, the body and brain begin adapting in ways that are hard to reverse. What starts as occasional use often shifts into something that demands more—higher doses, increased frequency, and consequences that weren’t visible at the beginning.
Brain chemistry changes with chronic ketamine use. The dissociative effects that once felt temporary start lingering between doses. Memory problems become noticeable—forgotten conversations, missed appointments, difficulty recalling information that was once easily accessible. Cognitive function slows down. Tasks that require focus and problem-solving become frustrating or overwhelming. These aren’t just “foggy” moments—they’re signs the brain is functioning differently now.
The emotional landscape shifts too. Many people experience deepening feelings of disconnection or emotional flatness between uses. Dissociation, that feeling of being separated from oneself or reality, can persist even during periods of sobriety. Emotional numbness or detachment from relationships that once mattered becomes more common. This isn’t a character flaw—it’s what happens when ketamine repeatedly disrupts the neural pathways that regulate emotional connection and behavioral wellness.
Physically, chronic ketamine use creates damage that’s harder to ignore. The bladder takes significant impact—painful urination, frequent urgency, and in severe cases, permanent bladder damage that requires medical intervention. Kidney function declines as the body struggles to process regular ketamine use. Stomach pain, liver stress, and cardiovascular strain add to the physical toll.
Tolerance builds steadily, meaning higher doses are needed to achieve the same effects that smaller amounts once produced. This escalation isn’t about willpower—it’s the body adapting to the substance. The cycle becomes self-reinforcing: increased use to chase the feeling creates more tolerance, which demands even higher doses.
Daily life starts reflecting these changes. Work performance suffers. Relationships strain under the weight of absence, even when someone is physically present. The gap between past functioning and current reality widens, and bridging it without professional support becomes increasingly difficult. This is where Cenikor’s continuum of care—from medical detox through residential treatment and outpatient support—provides the structured environment needed to interrupt the cycle and begin rebuilding physical health and daily functioning.
How Ketamine Rewires Your Brain Over Time: Long Term Effects of Ketamine Use
Memory Loss and Cognitive Decline
What you’ll learn: In this section, you’ll see how the long term effects of ketamine use can chip away at memory and mental sharpness—often so gradually that changes feel like normal forgetfulness or stress. You’ll know you’re ready for the next level when you can spot the difference between fleeting lapses and the deeper, persistent cognitive shifts linked to repeated ketamine exposure.
Memory loss isn’t just a side effect of occasional use—it’s a core risk for anyone using ketamine chronically. Research shows that long-term ketamine use damages the very brain regions that store and retrieve information, including the hippocampus and prefrontal cortex. This damage can result in working memory problems, trouble learning new information, and difficulty recalling names, appointments, or even major life events.1
Cognitive decline goes beyond memory. Chronic users often report slower problem-solving, poor focus, and increased mental fatigue. These changes are backed by neuroimaging studies, which have found that loss of gray and white matter leads directly to measurable drops in executive function and processing speed. One key finding: executive dysfunction from ketamine isn’t just frustrating—it’s linked to higher treatment dropout rates and greater barriers to recovery.1,10
Practice This: Try tracking your ability to remember details or keep up with conversations over a week. If you notice more frequent lapses or mental fog that doesn’t clear with rest, these may be early signs of persistent cognitive injury.
Next, we’ll look at how ketamine’s impact on the brain also disrupts emotional stability and can trigger dissociation.
Emotional Regulation and Dissociation
What you’ll learn: In this section, you’ll understand how the long term effects of ketamine use disrupt your ability to manage emotions and cause dissociation—a sense of detachment from reality or your own body. You’ll know you’re ready for the next level when you can identify signs of emotional numbness, mood swings, or moments where reality feels out of reach, and connect them to sustained ketamine exposure.
Chronic ketamine use doesn’t just cloud memory; it slowly erodes the brain’s emotional regulation systems. You might notice that situations which once felt manageable now trigger intense mood swings, irritability, or a persistent sense of emotional flatness. Studies show that repeated ketamine exposure can shrink and disconnect the brain regions responsible for processing emotions and self-awareness, making it harder to recover from stress or feel connected to others.1
One of the lesser-known but deeply unsettling long term effects of ketamine use is dissociation. This can show up as feeling like you’re watching life from outside your body, or as if the world around you has gone dull and unreal. Over time, these episodes may become more frequent and longer-lasting, interfering with relationships, work, and your sense of self.1
Practice This: Take a moment to jot down times when you’ve felt emotionally numb or disconnected from your surroundings. Noticing these patterns is the first step toward regaining emotional stability.
You’re making real progress if you can spot these subtle shifts—not just in yourself, but in clients or peers as well. Next, we’ll examine how ketamine’s physical damage often builds up without clear warning signs.
Physical Damage That Builds Silently
Bladder and Kidney Destruction
What you’ll learn: In this section, you’ll discover how the long term effects of ketamine use devastate the urinary system—often with little warning until significant damage is done. You’ll know you’re ready for the next section when you can identify the signs and complications of ketamine-induced bladder and kidney injury, and understand why early recognition is critical for preserving long-term health.
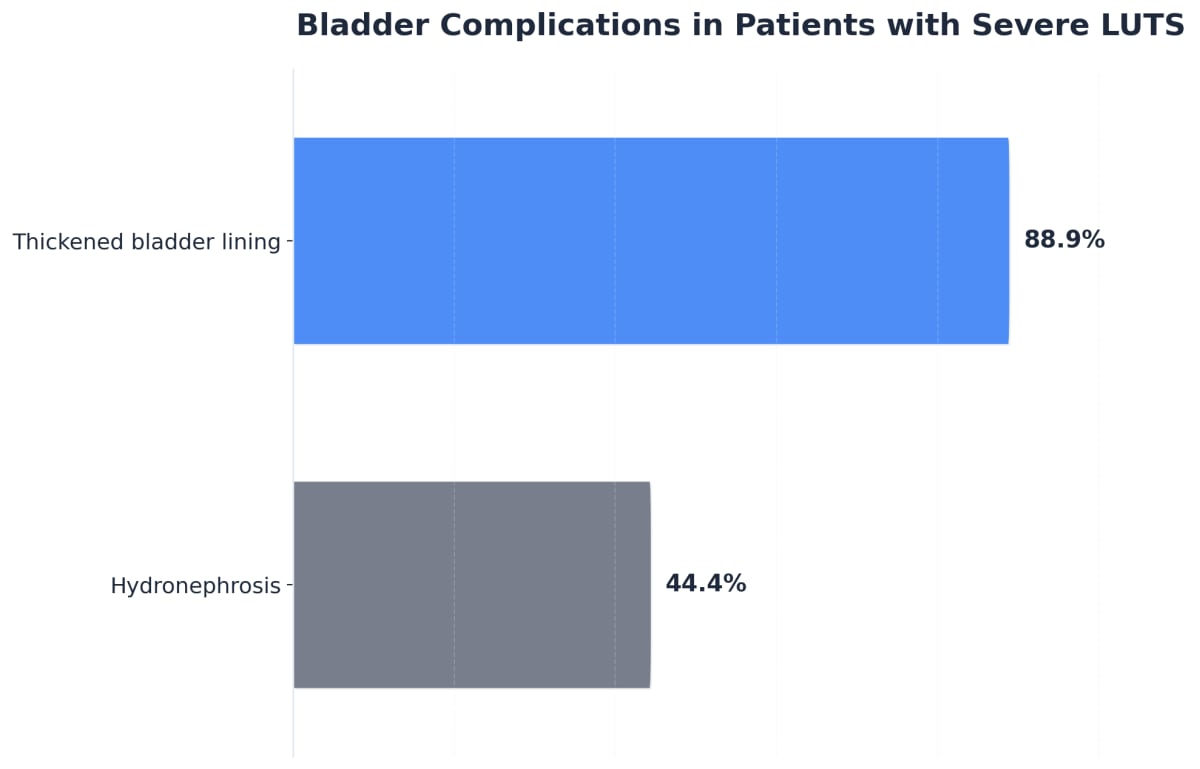
Bladder and kidney destruction is one of the most distinct and alarming consequences of chronic ketamine use. Even at recreational doses, ketamine can inflame and scar the bladder lining, sometimes causing symptoms in as little as a few months of regular use. Roughly 25% of recreational users report urinary symptoms such as urgency, pain, or blood in the urine, and the risk increases sharply with higher doses and frequency. Over time, the bladder loses its ability to stretch and store urine, resulting in frequent urination, incontinence, and severe pain—symptoms that can be life-altering for people in active addiction or in their care.6
But the damage doesn’t stop at the bladder. As scarring and inflammation progress, they can block urine flow, causing urine to back up into the kidneys—a condition called hydronephrosis. Studies have shown that up to 51% of patients with ketamine-related uropathy develop hydronephrosis, which can lead to permanent kidney damage and even kidney failure if left unaddressed. Secondary infections are also common, with up to 30% of cases presenting with symptoms that mimic standard urinary tract infections, potentially delaying correct diagnosis and care.5
Practice This: Start a log of urinary symptoms—frequency, pain, changes in color or odor—in clients or yourself. Early tracking can spot red flags before irreversible damage sets in.
You’re making meaningful progress when you can connect subtle urinary complaints to the possibility of ketamine-related injury. Next, let’s examine how long-term use can quietly harm the liver, heart, and digestive system.
Liver, Heart, and Gastrointestinal Harm
What you’ll learn: Here, you’ll see how the long term effects of ketamine use go far beyond the urinary tract—damaging your liver, heart, and digestive system in ways that are easy to miss until serious complications arise. You’ll know you’re ready for the next section when you can identify at least two warning signs of organ involvement and understand how subtle symptoms add up over time.
Liver injury is a lesser-known but real risk for chronic ketamine users. Over time, ketamine can inflame or scar the bile ducts, leading to cholangiopathy—a condition that disrupts the flow of bile and can cause jaundice, abdominal pain, and even permanent liver damage. One study found that nearly 10% of chronic users developed liver injury, often showing abnormal liver enzymes and fibrosis. At higher doses, liver enzyme activity can skyrocket up to 14 times normal levels, raising the risk of more severe complications.7
Your heart isn’t immune, either. Chronic ketamine use weakens the heart’s ability to pump, sometimes causing arrhythmias or even acute heart failure—especially in those with preexisting heart issues. Studies have documented a 21% drop in cardiac performance during ketamine infusion, highlighting just how quietly these risks can build.2
Digestive problems are also common but often overlooked. Up to 75% of long-term users report symptoms like chronic stomach pain, nausea, or rapid weight loss due to inflammation and slowed gut movement. These issues can drain energy, disrupt nutrition, and make daily functioning much harder.4
Practice This: Track unexplained abdominal pain, fatigue, or episodes of rapid heartbeat in yourself or clients. Early recognition makes a difference.
By connecting these subtle symptoms to the long term effects of ketamine use, you’re better equipped to spot damage early. Next, we’ll look at how tolerance and dependence can spiral, making daily life harder to manage.
When Daily Life Starts Breaking Down
Tolerance, Escalation, and Dependence
What you’ll learn: By the end of this section, you’ll understand how tolerance, escalation, and dependence develop with chronic ketamine use—and why these patterns make it so hard to regain control without support. You’ll know you’re ready for the next level when you can recognize the early signs of increasing use, the challenges of cutting back, and how these processes contribute to the long term effects of ketamine use.
Tolerance builds quietly. Over time, the same dose of ketamine brings less relief or euphoria, prompting you to use more just to feel “normal.” This isn’t about weak willpower—it’s a direct result of your brain adapting to constant exposure. As tolerance rises, escalation often follows: doses get larger, the intervals between use shrink, and it becomes harder to imagine getting through a day without it. Research shows that the longer and more frequently you use, the more deeply ketamine rewires the brain’s reward circuits, cementing patterns that are tough to break.1
Dependence can sneak up on anyone, even experienced professionals. Suddenly, cutting back triggers cravings, irritability, or physical discomfort. These withdrawal-like symptoms are your body’s alarm system, signaling real changes in brain chemistry—not just habit or preference.12
Practice This: Look back at your own use or clients you work with. Note any patterns of needing more over time, or failed attempts to reduce use. Recognizing these trends early can make all the difference.
When you can spot tolerance and escalation before full dependence sets in, you’re already a step ahead. Up next, let’s see how these changes start to fracture work, relationships, and personal identity.
Impact on Work, Relationships, and Identity
What you’ll learn: By the end of this section, you’ll see how the long term effects of ketamine use gradually disrupt your career, relationships, and even your sense of self—often before you realize what’s happening. You’ll know you’re ready for the next level when you can describe at least two concrete ways chronic ketamine use impacts daily functioning both at work and at home.
The breakdown of daily life isn’t always dramatic at first. Subtle cognitive changes—like memory lapses or difficulty focusing—can make it harder to keep up with deadlines, client needs, or basic professional responsibilities. Research has shown that executive dysfunction from chronic ketamine use is closely linked to missed work, poor decision-making, and even job loss, especially among those in high-pressure roles.10
Relationships often suffer next. Mood swings, emotional numbness, and dissociation can leave partners, friends, or colleagues feeling pushed away. Over time, trust erodes and communication breaks down, making isolation and conflict more common. Many users report losing touch with their core values, ambitions, or identity as the drug becomes central to daily routine.1
Practice This: Reflect on recent interactions—have you noticed increased misunderstandings or withdrawal from loved ones or co-workers? Document a specific example. Recognizing these patterns is a key step toward regaining wellness and connection.
If you can link changes in work performance or relationships to ongoing ketamine use, you’re ready to explore why stopping on your own is often so difficult.
Frequently Asked Questions
Can bladder damage from ketamine use be reversed if I stop now?
Stopping ketamine use as soon as possible offers the best chance for your bladder to recover. Research shows that early intervention can lead to significant improvement in symptoms like pain, urgency, and frequent urination—especially if scarring or severe shrinkage hasn’t set in yet. In many cases, people who stop using ketamine early see stabilization or even partial reversal of bladder inflammation and function over several months. However, if use has continued for a long time or symptoms are severe, some changes—like fibrosis or a thickened bladder wall—may be permanent and require ongoing management. Taking action now can help prevent further damage and improve your quality of life.6
How does ketamine damage differ from other substance-related health problems?
Ketamine’s long-term damage stands out from other substances because of its severe impact on the urinary system. Unlike opioids or stimulants, ketamine can rapidly inflame and scar the bladder, leading to cystitis, ulcers, and even irreversible shrinkage—a pattern rarely seen with other drugs. Chronic use also raises the risk of kidney damage due to urine backup and persistent inflammation. While other substances often target the liver or heart, ketamine’s dose-dependent urinary harm is unique and can develop even in recreational users. Recognizing this distinct risk helps you catch complications early and tailor your approach to care.5,6
Why do I need professional treatment if ketamine isn’t considered as addictive as other drugs?
Even though ketamine may not cause intense cravings like opioids or stimulants, the long term effects of ketamine use are still serious and often require professional care to address. Repeated use can rewire your brain’s reward system, making it incredibly difficult to cut back without structured support—especially as tolerance and dependence grow. Many people underestimate how quickly cognitive decline, emotional instability, and organ damage can set in, sometimes progressing even after use stops. Professional treatment offers monitoring, medical guidance, and ongoing support that self-managed efforts typically can’t provide, greatly improving your chances of lasting wellness and recovery.1,11,12
What medical tests should I expect when seeking treatment for ketamine-related damage?
When starting treatment for ketamine-related damage, you can expect a thorough medical evaluation focused on the organs ketamine most often affects. Typical tests include urine analysis and ultrasound of the bladder and kidneys to detect cystitis, hydronephrosis, or other urinary tract changes. Blood tests will assess kidney and liver function, looking for elevated creatinine or abnormal liver enzymes that signal ongoing injury. Some providers may order imaging studies—like CT or MRI scans—if severe symptoms are present, or recommend heart monitoring if there are signs of cardiovascular involvement. This comprehensive approach helps catch the long term effects of ketamine use early and guide your care plan.2,5,6,7
How long does it take for cognitive function to improve after stopping ketamine?
Cognitive recovery after stopping ketamine depends on how long and how heavily you’ve used, but some improvement is possible—even if changes felt permanent at first. Research shows that memory, attention, and executive function can gradually rebound over weeks to months, especially with early intervention and ongoing support. For many, the first signs of clearer thinking show up within the first three months, though full recovery may take longer or remain incomplete if use was prolonged. Staying engaged in wellness routines and tracking progress can help reinforce new habits as your brain repairs itself. If symptoms linger, don’t lose hope—continued improvement is still possible with time and support.1,10
Are there specific warning signs that kidney damage has already started?
Yes, there are several warning signs that kidney damage from ketamine use may have already started. Early symptoms often include lower back pain, swelling in the ankles or feet, or a noticeable drop in urination. Some people also develop high blood pressure or experience fatigue that doesn’t improve with rest. In advanced cases, blood tests may show elevated creatinine or a reduced glomerular filtration rate—markers of declining kidney function. Swelling of the kidneys (hydronephrosis) is found in about half of people with ketamine-related urinary tract problems, and this can progress even if bladder symptoms seem mild. If you notice these changes, prompt medical evaluation is crucial.5
Conclusion
Why Stopping Alone Is Difficult
Ketamine changes how your brain functions—and those changes don’t just disappear when you decide to quit. Your brain has adapted to the drug’s presence, building tolerance and dependence that make stopping on your own incredibly challenging. When you try to cut back or quit, you may face withdrawal symptoms like restlessness, confusion, intense cravings, and cognitive fog that can last for weeks. These aren’t signs of failure—they’re neurological responses that require professional support.
The physical complications add another layer of difficulty. If you’re already experiencing bladder pain, urinary problems, or kidney issues, stopping abruptly without medical supervision can be risky. Your body needs time to stabilize, and some symptoms may actually worsen before they improve. That’s why medical detox and ongoing clinical support aren’t just helpful—they’re often necessary to safely navigate the early stages of recovery and address the physical damage that’s already occurred.
How Cenikor Helps Stabilize and Rebuild
Recovery from ketamine abuse requires more than willpower—it requires the right level of care at the right time. Cenikor offers a full continuum of evidence-based treatment designed to meet you wherever you are in your journey. Starting with medical detoxification to safely manage withdrawal, you can transition through residential treatment for intensive stabilization, partial hospitalization programs (PHP) for structured daily support, and outpatient services that fit around your life as you rebuild.
What sets Cenikor apart is both the depth of care and the accessibility. As a designated Center of Excellence by Evernorth Behavioral Health (Cigna), Cenikor maintains the highest standards of evidence-based treatment while operating as a nonprofit—which means affordability is built into the model, not an afterthought. We accept over 30 major insurance carriers and offer flexible payment options, so cost doesn’t have to be a barrier to getting help. With nearly 60 years of experience serving Texas and New Mexico, Cenikor provides medication-assisted treatment when appropriate, custom treatment plans tailored to your specific needs, and recovery housing to support your transition back to independent living.
Conclusion
The long-term effects of ketamine abuse aren’t just about what happens in the moment—they’re about what builds up over time. The damage to your bladder, kidneys, brain, and overall wellness doesn’t always announce itself right away, but it becomes harder to ignore as use continues. You might notice memory gaps, trouble focusing, or physical pain that won’t go away. These aren’t signs of weakness—they’re your body asking for help.
The good news? You don’t have to face this alone. Recovery is possible, and the earlier you reach out, the more you can protect yourself from further harm. Whether you’re just starting to see the impact or you’ve been struggling for a while, Cenikor offers evidence-based treatment designed to meet you where you are. As a nonprofit with nearly 60 years of experience, we provide affordable, comprehensive care that treats you with dignity and gives you real tools for lasting change. Taking that first step is brave—and it matters. Call Cenikor today to speak with an admissions specialist who can help you understand your options and start your path to recovery.
References
- Brain Changes Associated With Long-Term Ketamine Abuse – PMC. https://pmc.ncbi.nlm.nih.gov/articles/PMC8972190/
- Ketamine Induced Acute Systolic Heart Failure – PMC. https://pmc.ncbi.nlm.nih.gov/articles/PMC11152225/
- Brain Changes Associated With Long-Term Ketamine Abuse – Frontiers. https://www.frontiersin.org/journals/neuroanatomy/articles/10.3389/fnana.2022.795231/full
- Multiorgan Dysfunction Related to Chronic Ketamine Abuse – PMC. https://pmc.ncbi.nlm.nih.gov/articles/PMC4059572/
- Ketamine Impact on Kidney Health – PMC. https://pmc.ncbi.nlm.nih.gov/articles/PMC11531648/
- Ketamine-Induced Cystitis: A Comprehensive Review – PMC. https://pmc.ncbi.nlm.nih.gov/articles/PMC9476224/
- Ketamine Hepatotoxicity – PMC. https://pmc.ncbi.nlm.nih.gov/articles/PMC12134908/
- Ketamine Induced Acute Systolic Heart Failure – PMC. https://pmc.ncbi.nlm.nih.gov/articles/PMC11152225/
- Ketamine Induces Toxicity in Human Neurons – PMC. https://pmc.ncbi.nlm.nih.gov/articles/PMC3684944/
- Cognitive Impairment in Chronic Ketamine Abusers – PubMed. https://pubmed.ncbi.nlm.nih.gov/32763531/
- Early Intervention, Treatment, and Management – NIH. https://www.ncbi.nlm.nih.gov/books/NBK424859/
- Fast Bursts of Dopamine Limit Ketamine Addiction – PMC. https://pmc.ncbi.nlm.nih.gov/articles/PMC10342185/
Recovery Built for Real Life
Recovery doesn't have to feel out of reach. At Cenikor, we provide practical, affordable care designed for real life—whether you're navigating substance use, supporting a loved one, or helping someone find the right level of care.
Explore Your Options

